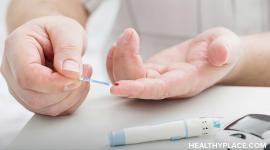
What is the Difference Between Type 1 and Type 2 Diabetes?
There is a significant difference between type 1 and type 2 diabetes. Of course, these diseases are two types of diabetes and thus share similarities. Here we’ll explore the similarities and differences between type 1 and type 2 diabetes to help you evaluate which type of diabetes might apply to you or a loved one if you’re concerned about diabetes ("Diabetes Symptoms and Signs in Adults, Men, Women and Children").
Type 1 and Type 2: Both are Diabetes
Diabetes is a metabolic disorder, which means that there’s a problem with the way the body metabolizes glucose into energy ("What Is Diabetes?"). Glucose is created during digestion when carbohydrates you’ve eaten are broken down into sugar (glucose). Glucose enters the bloodstream where it travels to the cells of your body. Your cells need glucose for energy, but glucose can’t get into the cells on its own. It needs insulin, which is a hormone made in an organ called the pancreas. Under normal circumstances, insulin goes to work when blood glucose levels rise, and it unlocks the cells so glucose can get out of the blood and into cells where it can be used as energy.
In diabetes, there is a problem with insulin so that glucose can’t enter the cells of the body and remains stranded in the bloodstream. Glucose levels continue to rise, and the result is hyperglycemia, or high blood sugar (high blood glucose).
Diabetes types 1 and 2 both involve high blood glucose levels and are metabolic disorders. If it were this simple, though, the disease would just be called hyperglycemia and there wouldn’t be different types of diabetes. Everything just described does occur in diabetes, but the picture is incomplete.
Difference Between Type 1 and Type 2 Diabetes: Insulin
The key difference between type 1 and type 2 diabetes involves what happens with insulin. As we’ve seen, both types of diabetes are disorders of metabolism. Type 2 diabetes is only a metabolic disorder, while type 1 diabetes is also an autoimmune disorder.
All autoimmune diseases involve the immune system turning on its own body, attacking parts of the person’s systems. In the case of type 1 diabetes, the immune system produces cells called autoantibodies that attack the beta cells in the pancreas.
As a result of the immune system’s behavior, the beta cells are destroyed and the pancreas loses its ability to produce insulin. The person’s body cannot make the insulin it needs to move blood glucose into the cells for energy. The disease is permanent because after the immune system destroys something—in this case insulin-producing beta cells—it’s permanently gone.
Insulin is also a problem in type 2 diabetes, but in a different way. In type 2, the body often makes enough insulin and should be able to move blood sugar into cells. However, something prevents that from happening by resisting insulin’s actions. This is known as insulin resistance. There is insulin, but the body isn’t using it efficiently, and hyperglycemia develops.
Sometimes in type 2 diabetes, the body stops producing enough insulin to work correctly. Many times, this happens because the pancreas has been working on overdrive to compensate for insulin resistance. Over time, the pancreas experiences burnout and will continue to produce insulin, but not as much as needed.
The difference between Type 1 and Type 2 Diabetes: Who Gets These Diseases?
Type 1 diabetes is much less common than type 2 diabetes. Of all cases of type 1 and type 2 diabetes, type 1 accounts for approximately 5-10 percent, and type 2 makes up all the rest.
Anyone can develop either type of diabetes at any time, although the two types of diabetes each has a higher likelihood in different populations.
Type 1 diabetes:
- Tends to develop in younger people, with half of all cases diagnosed by the early teens and many others by the 20’s ("What Are Type 1 Diabetes Symptoms and Signs?")
- Has unpredictable, uncontrollable risk factors that are still poorly understood and may involve genetics, the environment, and autoimmune aspects that are hard to pinpoint
- Requires daily insulin injections
Type 2 diabetes:
- Tends to increase with age, with diagnoses increasing as people age beyond 45 ("What Are Type 2 Diabetes Symptoms? ")
- Has risk factors largely involving lifestyle: people with poor diet, low activity levels, and who are overweight have the highest risk of developing type 2 diabetes.
- Treatable with lifestyle management and, in some cases, a diabetes medication that may or may not include insulin
There are indeed differences between type 1 and type 2 diabetes. A key similarity is that while there is no cure for either type, both types can be treated and managed so people can enjoy life.
APA Reference
Peterson, T.
(2022, January 4). What is the Difference Between Type 1 and Type 2 Diabetes?, HealthyPlace. Retrieved
on 2026, May 16 from https://www.healthyplace.com/diabetes/main/what-is-the-difference-between-type-1-and-type-2-diabetes