Feeling safe after enduring trauma or developing posttraumatic stress disorder (PSTD) can be a challenge. Growing up, I had a persistent uneasy feeling in my gut that manifested as a constant stomach ache. After being sexually assaulted by another (though older) child, I found myself unable to feel at ease in my own body. I worried not only about my personal safety but also my family's — especially since the boy threatened to hurt me and my loved ones if I told anyone what he did to me. Feeling safe with PTSD turned out to be very hard.
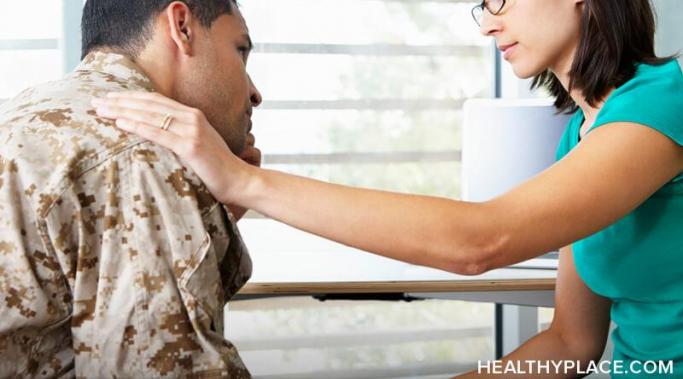
PTSD Treatments
I realize I need to be my own hero, but it's hard. As someone with a highly self-critical brain and a history of trauma and posttraumatic stress disorder (PTSD), I often struggle to take control of my own healing. In my experience, it's tempting to turn to others during difficult moments (which is completely okay and necessary sometimes) rather than turning inward and finding my own resilience. Self-sabotage takes merit over self-love and self-care, and before I know it, I'm spiraling into anxiety and grief, looking elsewhere for someone to do the work for me — to be my hero.
Talking about trauma is not an easy feat. But if you're constantly reliving a specific traumatic event or cycling through negative thoughts surrounding the trauma, confiding in a trusted loved one can help you feel less alone. A supportive community is integral to trauma recovery, and you don't have to go through it all alone. You can tell about your trauma.
Dealing with posttraumatic stress disorder (PTSD) at work can be stressful. Navigating flashbacks, panic attacks, and hypervigilance is difficult in any setting, but managing these symptoms in a workplace can feel impossible. When you're constantly worrying about judgment from your coworkers and peers, it can be hard to focus on the job at hand.
Grounding techniques are a valuable coping tool for people suffering from posttraumatic stress disorder (PTSD). At its core, PTSD is a disorder that keeps people stuck in the past. Grounding techniques, on the other hand, help people with PTSD connect with the present. Finding grounding techniques that work for my PTSD symptoms has been a journey. Grounding is a very personal experience, and what works for other people doesn't always work for me. Thankfully, there are plenty of techniques to choose from when it comes to grounding yourself.
Life is tough at the moment. Every day that passes by seems to be filled with anxiety after anxiety, and there is no clear end in sight. COVID-19 has thrown all our lives into disarray, and coping with mental health issues is harder than ever. Being stuck at home is undoubtedly difficult for everyone. Human connection is an essential part of life, and being unable to connect with friends and family members because of the coronavirus is taking a toll on all of us. But for people with serious mental illnesses such as posttraumatic stress disorder (PTSD), social isolation can present unique challenges.
Nightmares are one of the most common symptoms of posttraumatic stress disorder (PTSD). While most people experience a nightmare or two in their lifetime, up to 72% of people suffering from PTSD develop recurring nightmares as a result of the disorder. I am one of those people. I started experiencing nightmares as a result of PTSD when I was sixteen. Almost eight years later, I still get them every time I close my eyes to sleep. Coping with daily nightmares (and the poor sleep quality that can result) has been difficult, but I have found ways to manage them over time.
Posttraumatic stress disorder (PTSD) can get worse before it gets better when you start therapy. Find out why that's normal and how to handle it.
Posttraumatic stress disorder (PTSD) is exhausting. I often describe the disorder as a brain at war with itself, fighting and pulling different parts of your mind in all directions. The thoughts, worries, and instincts circling through your head can get so loud at times that it makes you want to cover your ears.
Today I want to talk about why it's so difficult to follow through on New Year's resolutions when you have posttraumatic stress disorder (PTSD).